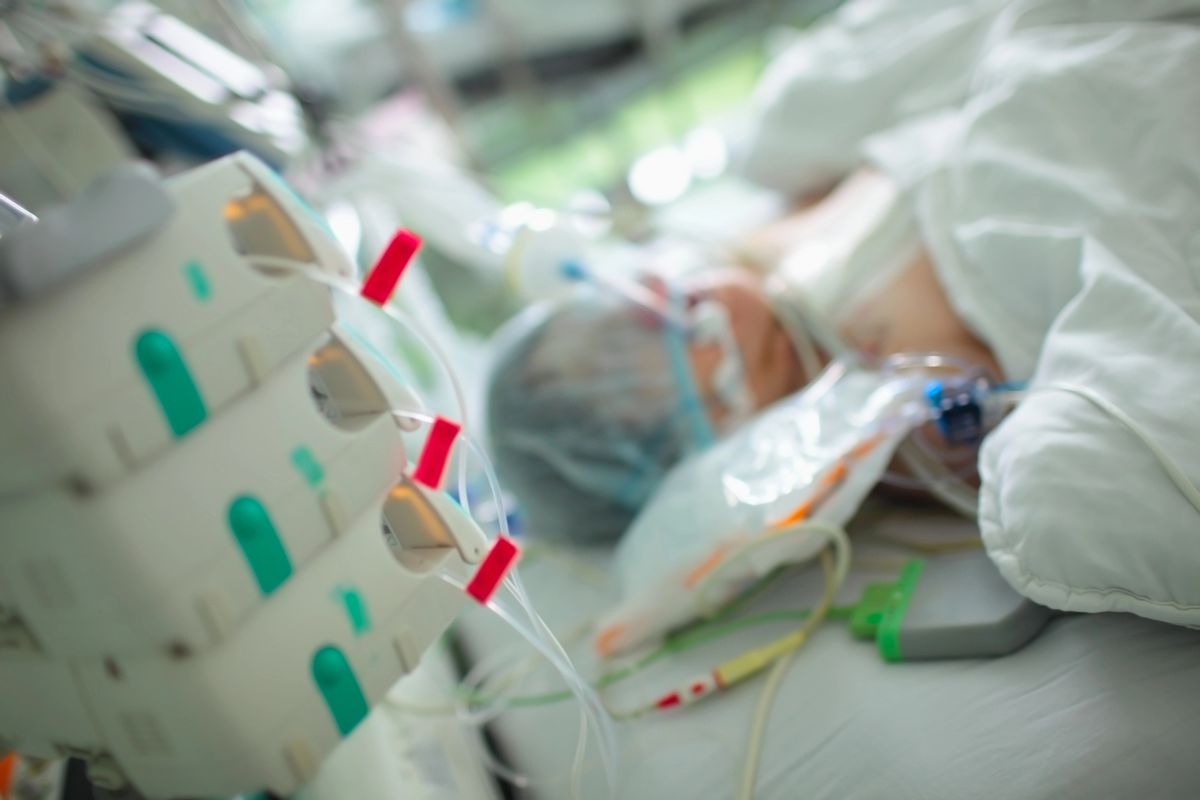
A coma state, from a medical point of view, is a profound state of unconsciousness in which the patient does not respond to external stimuli and shows no signs of conscious activity. It is the result of severe brain damage, which can be caused by a variety of factors, such as head injuries, stroke, brain tumours, brain infections, or chemical and drug poisoning.
Coma can result from direct damage to brain structures responsible for consciousness and alertness, such as the brainstem and networks that activate the reticular system. It can also result from systemic disorders that affect brain function, such as extreme metabolic disturbances, hypoxia (oxygen deficiency) or poisoning.
Diagnosis of coma requires a comprehensive medical assessment, including a neurological examination that assesses level of consciousness, responses to stimuli and basic vital functions. Scales such as the Glasgow Response Scale (GCS), which assesses the depth of coma based on ocular, verbal and motor responses, are often used to assess the patient's condition.
It is important to distinguish the coma state from other states of altered consciousness, such as the vegetative state (VS) or the state of minimal consciousness (MCS). A vegetative state is characterised by a lack of awareness of self and surroundings while maintaining sleep-wake cycles, whereas a state of minimal consciousness is associated with minimal but noticeable signs of awareness
Empathy and communication
Empathy and non-verbal forms of communication are fundamental in the care of comatose patients, playing a key role in the healing process and influencing the way medical staff and families perceive and approach patient care. These aspects of a humanistic approach to medicine not only facilitate a deeper bond with the patient, but can also have a positive impact on health.
Empathy in the context of caring for comatose patients manifests itself primarily through a compassionate and attentive approach to the patient and their family. It is the ability to understand and empathise with their situation, which is extremely important as these patients are unable to express their needs and feelings in traditional ways. An empathic approach helps medical staff to better understand not only the physical but also the emotional needs of the patient, which is key to providing holistic care.
Non-verbal Communication with the Patient
Non-verbal forms of communication, such as touch, tone of voice or even presence at the patient's bedside, can convey support, safety and care. Although comatose patients do not react consciously, some studies suggest that they may sense the presence of loved ones and medical staff on a subconscious level. Practices such as talking to the patient during procedures, holding his or her hand or maintaining eye contact (where possible) may help to maintain a sense of human presence and connection.
Empathy and non-verbal communication not only have a symbolic dimension, but can also influence treatment outcomes. Although direct evidence of the impact of these practices on health outcomes is difficult to determine conclusively, it has been observed that positive attitudes and emotional support can improve a patient's overall condition, including stabilising vital functions or even reducing the length of time a patient remains in a comatose state.
The humanistic approach to coma care emphasises that every patient, regardless of their state of consciousness, deserves respect, dignity and care. It is a reminder that behind every medical aspect is a human being whose values, experiences and emotional needs matter. This approach not only affects the quality of care, but also the public's perception of patients, promoting more sensitive and empathetic standards in medicine.
The conclusion is that empathy and non-verbal communication are indispensable elements in the care of comatose patients, emphasising the humanistic dimension of medicine. These practices not only strengthen the bond between patient and carer, but can also have a real impact on the treatment process, raising the standards of medical care and promoting the dignity of each patient.Beginning form